 
This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. The cookies is used to store the user consent for the cookies in the category "Necessary". The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". The cookie is used to store the user consent for the cookies in the category "Analytics". These cookies ensure basic functionalities and security features of the website, anonymously. Necessary cookies are absolutely essential for the website to function properly. Non-union is less common, occurring in <1% cases. 
Malunion can also occur, especially if fractures treated non-operatively. The main significant risks of a tibial shaft fracture are compartment syndrome, ischaemic limb, or open fractures. ManagementĪssociated fractures of the fibula can usually be left alone as they heal very well once the tibial fracture has been stabilised. There may also be an associated fibula fracture, the location of which can correlate to the degree of energy causing the injury high energy mechanisms often result in a fibula fracture at the same level as the tibia, whilst low energy fractures often result in a fibula fracture at a different level. For any suspected a spiral fracture of the distal tibia, a CT scan is also required, to assess for a fracture of the posterior malleolus. 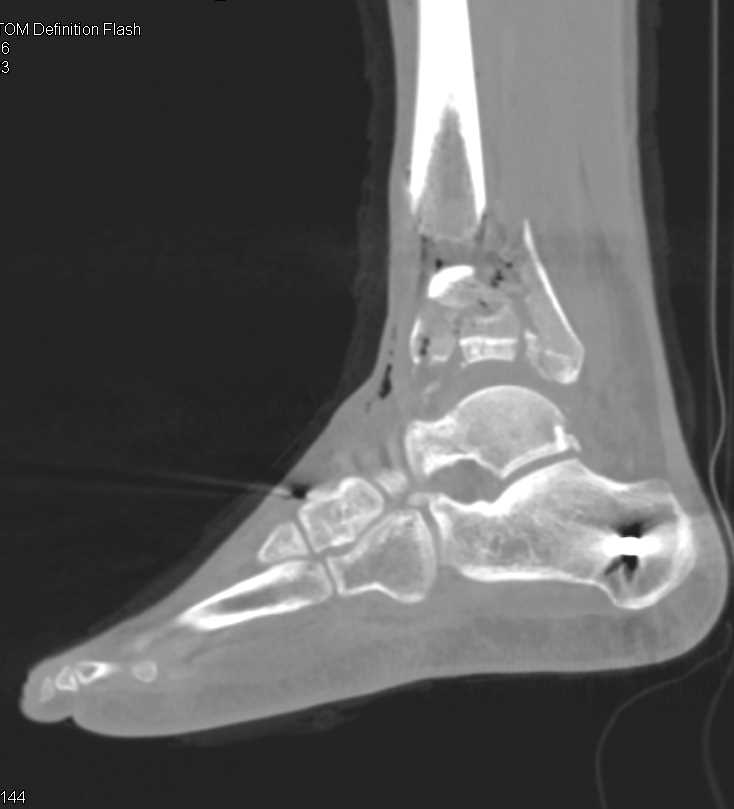
In cases of potential intra-articular extension, CT imaging will be indicated to evaluate. Imagingįull length antero-posterior (AP) and lateral plain film radiographs of the tibia and fibula should be requested, which need to also include the knee and ankle. Urgent bloods, including a coagulation and Group and Save, should be sent. Patients presenting following a major trauma should be investigated and managed as per the ATLS protocol. Figure 2 – An open tibial shaft fracture Differential DiagnosisĪs most cases present following a fall or trauma, differentials include tibial plateau fractures, ankle fractures, fibular fractures, or soft tissue injury. *Tibial shaft fractures are high risk for compartment syndrome, any pain out of proportion to the injury and pain significantly worse on passive stretch of the affected compartments is key A full neurovascular examination should be performed to assess for any concurrent vascular injury or peripheral nerve damage. On examination, there may be a clear deformity (such as angulation or malrotation) and significant swelling and bruising.Ĭareful inspection of the skin is essential to assess for the possibility of an open fracture, if not already evident (Fig. Patients will complain of severe pain* in the lower leg and an inability to weight bear. Patients will present with a history of trauma, however obtaining an accurate description of the injury (including direct and indirect forces that occurred) can suggest potential associated soft tissue injuries or other fractures present. Figure 1 – The bony landmarks of the tibial shaft Clinical Features Those with multiple injuries may require temporary external fixation if they are not stable enough to undergo definitive surgery.Īssociated fractures of the fibula can usually be left alone as they heal very well once the tibial fracture has been stabilised. Particularly proximal or distal fractures, especially those which extend into the joint, may require open reduction internal fixation (ORIF) with locking plates. Post-operatively, patients are usually able to fully weight bear immediately. Intramedullary (IM) nailing is the most commonly used method of fixing tibial shaft fractures, providing a stable construct through a minimally invasive approach, with a high success rate. Non-operative management with a Sarmiento cast should be considered in closed stable tibial fractures and must be discussed with the patient as an alternative to operative intervention. Urgent operative intervention is required in the context of an acute compartment syndrome, an ischaemic limb, or an open fracture. Most tibial shaft fractures are managed surgically. Post-manipulation plain radiographs should be performed and the neurovascular status of the limb re-assessed and documented. The limb must be elevated immediately and closely monitored for signs of compartment syndrome. Any open fracture must be managed accordingly.įollowing reduction, an above knee backslab (in slight flexion at the knee and neutral dorsiflexion at the ankle) should be applied to control rotation. The tibia should be realigned as soon as possible, ideally in A&E under analgesia / conscious sedation whilst exact anatomical reduction is not required, the tibia should be brought approximately to length and rotation. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
